|
Unfortunately, all three ulcerative conditions have similar characteristics, and serologic testing is often the key to making the diagnosis. If a patient doesn't already have a diagnosis of rheumatoid, physicians also suspect Wegener's granulomatosus, a serious vasculitis or Mooren's ulcer, which is peripheral ulcerative keratitis of unknown etiology. When presented with a non-infectious peripheral ulcerative keratitis, however, first suspect rheumatoid arthritis or another autoimmune condition. "Scrape it, culture it and put the patient on antibiotics," says Dr. "None of the immune conditions cause a hypopyon, while the bacterial ones do." If there's a hy-popyon, corneal specialists say to proceed as if it's a bacterial infection until proven otherwise. "If the eye is red and painful, and there's peripheral thinning with an epithelial defect, then you first assess the de-fect's size, location and whether it's associated with a hypopyon," says Dr. Since several of the ul-cerative conditions have similar ap-pearances, it takes more diagnostic detective work to narrow down the cause in these cases. These are the presentations that ophthalmologists are more con-cerned about, as actual tissue is being lost. Patients can also present with peripheral thinning accompanied by ulceration and general inflammation. "If a perforation is imminent and the vision is significantly impaired, or you're worried about a spontaneous perf or a perforation occurring from mild trauma, you could do a graft," says Dr. Rapuano says that, though there's no treatment for the thinning, you can manage the astigmatism with glasses or, failing that, RGPs or hybrid lenses. 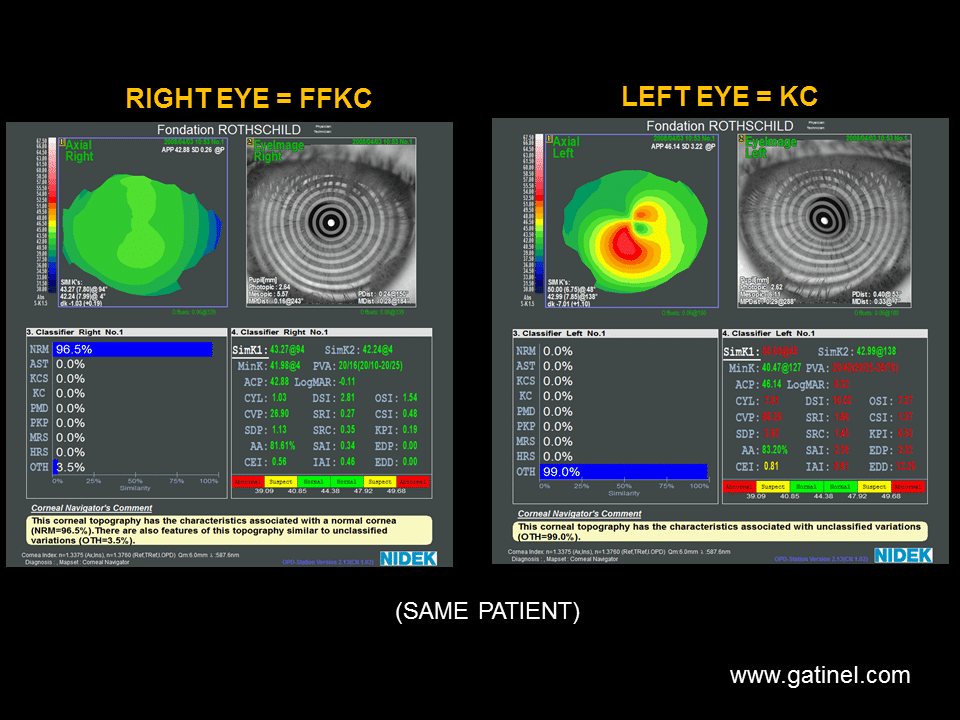
And, since it starts superiorly, the patient usually gets against-the-rule astigmatism." Dr. The thinning can be progressive, and can progress circumferentially or centrally. "However, the epithelium is also intact with this condition. "You'll see vascularization in addition to the thinning, often with a leading edge of lipid," explains Dr. It starts as a non-ulcerated area of thinning located superiorly, and it slowly progresses from there. This presents as a marginal furrow, usually bilateral, and is most common in men between 20 and 40 years of age. "Rarely, you'll need to do a corneal transplant." "For PMD, glasses sometimes help, though the management typically involves a rigid gas permeable contact lens or a hybrid lens like the Synergize," explains Dr. Though there's no redness, pain or inflammation, it causes significant irregular astigmatism, so the patient tends to complain of a slow, progressive worsening of vision." On topography, PMD will have an area of inferior steepening that resembles a crab claw, physicians note. "Some patients with pellucid can have severe thinning, usually inferiorly, within a couple of millimeters of the limbus. "However, where keratoconus tends to mean central or paracentral thinning, pellucid is peripheral," he says. This is a cousin to keratoconus, says Wills Eye Institute corneal specialist Christopher Rapuano. However, the hallmark signs of furrow degeneration are that the thinning, if it's present at all, is very shallow, non-progressive and isn't visually significant the eye is white and quiet, there's no vascularization and there's no possibility for perforation." As for management, physicians say furrows only need to be monitored at the patient's normal office visits, and no actual treatment is necessary. "It can sometimes be illusory because the arcus is there to thicken up the cornea," says Deepinder Dhaliwal, MD, director of cornea and external disease at the University of Pittsburgh Medical Center. This is a variety of peripheral thinning, typically between the limbus and the arcus senilis, that usually occurs in elderly patients. "If necessary, you can perform a temporary tarsorraphy." "In this case, the treatment is lubrication, maybe punctal occlusion, and a bandage contact lens," he says. In the absence of inflammation, one of the more likely causes of the thinning is a dell, or an area of non-wetting that thins and then breaks down, observes Sadeer Hannush, MD, a corneal specialist and attending surgeon at the Wills Eye Institute. If it's not, ophthalmologists say you can then look for the following causes: 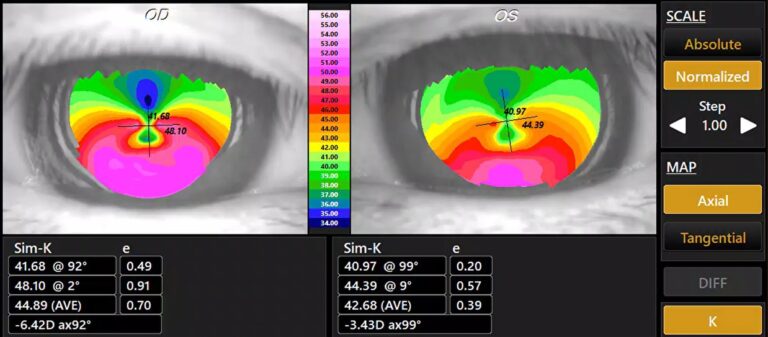
When a patient presents with some thinning in his corneal periphery, one of the first questions physicians ask is whether or not the eye is inflamed. In this article, corneal specialists explain how you can determine the cause of a patient's thinning peripheral cornea and start the proper treatment as quickly as possible. Possible causes abound, from autoimmune disease to staph hypersensitivity ulcers, and it's up to the ophthalmologist to sort them out and come up with the right one. 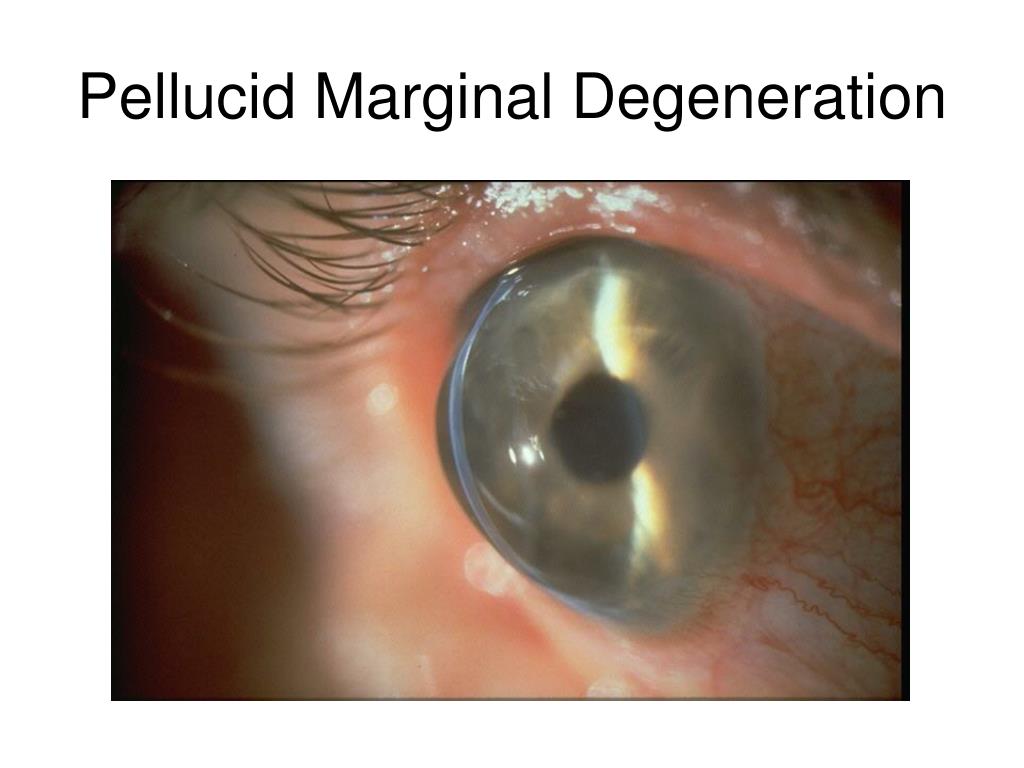
Everyone likes a good mystery, except when it involves finding the cause of peripheral corneal thinning.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
